PNAS: A New Study Revealed the Spread Path of Cell Transmission
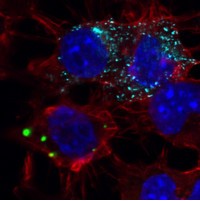
Microscope image of Nerve cells: Spreading of protein particles between cells.
According to a newly published lab study in the Proceedings of the National Academy of Sciences (PNAS), some protein particles can multiply and spread cell transmission. This finding would be meaningful for neuroscience research and application.
It is well known that many cognitive-related diseases are the result of nerve cell death. During the process, endogenous proteins will accumulate in brain. While the continue interconnection of these proteins eventually trigger the disease progression. But how these proteins act to each other? Do they work in chain?
In order to find the answer, scientists did the study with the help of cell cultures. They used cultured brain cells of mice; meanwhile they transferred a model protein into these cells to facilitate the protein production control. The blueprint of the molecule was extracted from yeast DNA. This protein does not exist in humans. They chose this particular protein because it had several properties that were relevant for the study: In its natural environment -- the yeast cell -- it is capable of forming replicating "aggregates" (for example, large protein particles). The protein deformed during this process. But scientists didn’t know whether something similar would happen in mammalian cells.
In further study, they didn’t gain the target protein on mouse. Then they tried to expose the cells to aggregates of the same protein. Suddenly, the proteins which had been in solution started building clumps. Once this reaction had been triggered the cells went on producing aggregates. The researchers noticed that these clumps spread into neighboring cells, where they initiated synthesis of further aggregates.
Propagation of aggregates was most effective between adjacent cells. In the study model, the protein particles are not released efficiently into the medium and assimilated by neighboring cells. The most effective transmission happens by direct cell-to-cell contact. It is possible that cells form protrusions and that aggregates move from one cell to the next through this connection.
Knowing the protein particles transmission is important as it may lead to new methods for treatment in clinical application.
Article Link: PNAS: A New Study Revealed the Spread Path of Cell Transmission

