IL-12 Family Ligands
Related Symbol Search List
Immunology Background
Available Resources for IL-12 Family Ligands Research
Creative BioMart is dedicated to providing a comprehensive range of products for the study of IL-12 family ligands. Our selection includes recombinant proteins, magnetic beads coupled with proteins, cell and tissue lysates, and more, all of which are of the highest quality to support researchers in their investigations. We understand that every research project is unique, so we offer customizable services to ensure that you receive the most suitable product for your specific needs.
In addition to our products, we also offer a wealth of information and resources on IL-12 family ligands. Our resources cover a range of topics, including pathways, protein function, interacting proteins, related articles, and research areas. These references are designed to deepen researchers' understanding of IL-12 family ligands and their importance in physiological processes.
Our Featured Products
| Cat.# | Product name | Species | Source (Host) | Tag |
|---|---|---|---|---|
| EBI3-287H | Recombinant Human EBI3, Fc tagged | Human | Human Cell | Fc |
| IL12A-315H | Recombinant Human IL12A, His tagged | Human | Human Cell | His |
| IL12-12H | Recombinant Human IL12 Protein, His-tagged | Human | HEK293 | His |
| IL12B-310H | Recombinant Human IL12B protein, Fc-tagged | Human | HEK293 | human/IgG1/Fc |
About IL-12 Family Ligands
The IL-12 family of cytokines comprises several ligands that play crucial roles in immune regulation and inflammation. Let's explore the different IL-12 family ligands:
IL-12 (Interleukin-12)
IL-12 is a heterodimeric cytokine composed of two subunits, IL-12A (p35) and IL-12B (p40). It is primarily produced by antigen-presenting cells, such as dendritic cells and macrophages. IL-12 plays a pivotal role in promoting immune responses against intracellular pathogens. It stimulates the differentiation of T cells into the Th1 subset, enhances the cytotoxic activity of natural killer (NK) cells, and induces the production of interferon-gamma (IFN-γ).
IL-23 (Interleukin-23)
IL-23 is another heterodimeric cytokine composed of two subunits, IL-23A (p19) and IL-12B (p40). It is predominantly produced by activated antigen-presenting cells. IL-23 plays a critical role in the differentiation and expansion of Th17 cells, a subset of T cells involved in immune responses against extracellular pathogens and implicated in autoimmune and inflammatory diseases. IL-23 promotes the production of pro-inflammatory cytokines, such as IL-17 and IL-22, which contribute to tissue inflammation.
IL-27 (Interleukin-27)
IL-27 is a heterodimeric cytokine composed of two subunits, IL-27p28 (p28) and EBI3 (Epstein-Barr virus-induced gene 3). It is produced by various cell types, including antigen-presenting cells. IL-27 has both pro-inflammatory and anti-inflammatory properties. It regulates immune responses by promoting the differentiation of regulatory T cells (Tregs), which play a role in immune tolerance and suppression of excessive inflammation. IL-27 also suppresses the production of pro-inflammatory cytokines and modulates the balance between Th1 and Th17 responses.
IL-35 (Interleukin-35)
IL-35 is a unique heterodimeric cytokine composed of two subunits, EBI3 and IL-12A (p35). It is predominantly produced by regulatory T cells (Tregs) and plays a crucial role in immune regulation. IL-35 has immunosuppressive properties and inhibits the proliferation and function of effector T cells. It promotes the generation of Tregs and contributes to immune tolerance and suppression of excessive inflammation.
These IL-12 family ligands bind to specific receptors on target cells, initiating intracellular signaling cascades that regulate immune responses, inflammation, and the differentiation of T cell subsets. The receptors involved in IL-12 family signaling include IL-12 receptor β1 (IL-12Rβ1), IL-23 receptor (IL-23R), IL-27 receptor α (IL-27Rα), and glycoprotein 130 (gp130). The activation of downstream signaling pathways, such as the Janus kinase (JAK)/signal transducer and activator of transcription (STAT) pathway, mediates the biological effects of IL-12 family cytokines.
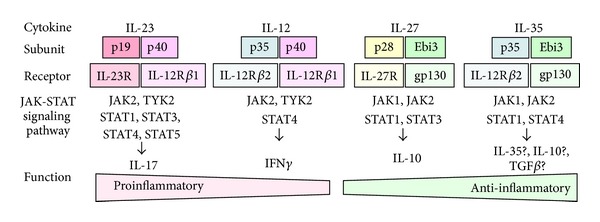 Fig.1 A schematic representation of IL-12 family cytokines and the corresponding receptors and JAK-STAT signaling pathways. (Shimizu J, et al., 2013)
Fig.1 A schematic representation of IL-12 family cytokines and the corresponding receptors and JAK-STAT signaling pathways. (Shimizu J, et al., 2013)
Importance of IL-12 Family Ligands in the Immune System
Regulation of T Cell Responses
IL-12 family ligands are involved in regulating T cell responses, specifically the differentiation and function of different T cell subsets. IL-12 promotes the differentiation of naive CD4+ T cells into Th1 cells, which are important for host defense against intracellular pathogens. IL-23 is crucial for the expansion and activation of Th17 cells, which contribute to immune responses against extracellular pathogens and are implicated in autoimmune diseases. IL-27 and IL-35 play roles in the regulation of regulatory T cells (Tregs), which are essential for immune tolerance and controlling excessive immune responses.
Modulation of Inflammatory Processes
IL-12 and IL-23 enhance the production of pro-inflammatory cytokines, such as IFN-γ, IL-17, and IL-22, which contribute to the inflammatory response and host defense mechanisms. IL-27 and IL-35, on the other hand, have anti-inflammatory properties and can suppress excessive inflammation by inhibiting pro-inflammatory cytokine production and promoting the generation of Tregs.
Host Defense against Pathogens
IL-12 and IL-23 promote the activation and cytotoxicity of NK cells, which play a vital role in the early defense against infected cells. Th1 and Th17 cells, induced by IL-12 and IL-23, respectively, produce cytokines that enhance the antimicrobial activities of phagocytes and recruit immune cells to sites of infection, aiding in pathogen clearance.
Autoimmunity and Immune-Mediated Disorders
Dysregulation of IL-12 family ligands has been associated with autoimmune diseases and immune-mediated disorders. Imbalances in Th1, Th17, and Treg responses, which are regulated by IL-12 family ligands, can contribute to the development and progression of autoimmune conditions. Understanding the role of IL-12 family ligands in these diseases provides insights into potential therapeutic targets for modulating immune responses.
Cancer Immunotherapy
IL-12, in particular, has been investigated for its potential to enhance anti-tumor immune responses. IL-12 administration can stimulate cytotoxic T lymphocytes (CTLs), NK cells, and Th1 responses, which are crucial for tumor cell recognition and elimination. IL-23 has also been implicated in tumor progression, highlighting its relevance in cancer biology.
In summary, IL-12 family ligands are essential for regulating immune responses, maintaining immune homeostasis, and influencing various pathological conditions. Their roles in T cell differentiation, inflammation, pathogen defense, autoimmune diseases, and cancer make them significant targets for therapeutic interventions and provide opportunities for advancing our understanding of the immune system.
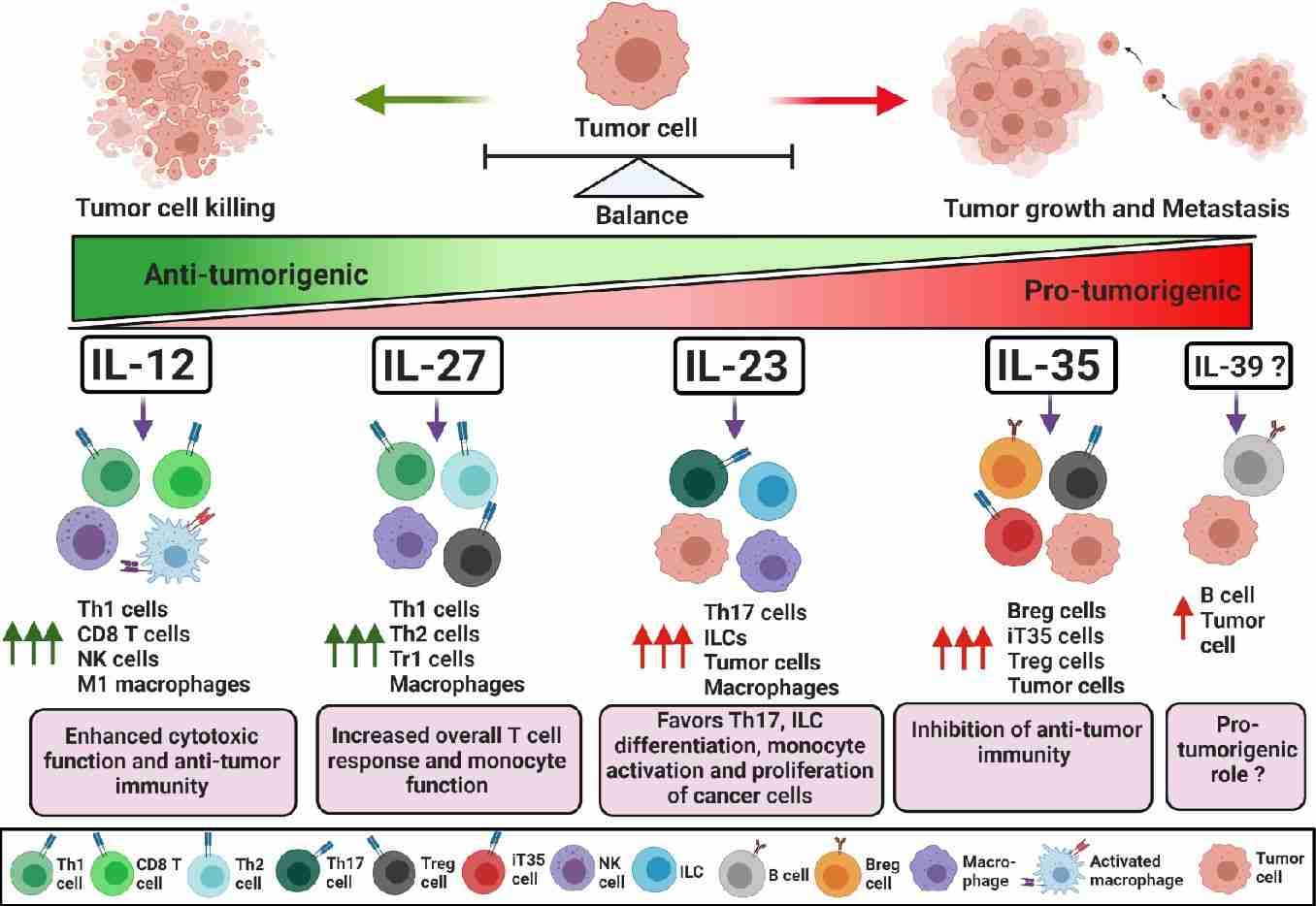 Fig.2 Role of IL-12 family cytokines in maintaining a balance between effector and regulatory immune responses in tumorigenesis. (Mirlekar B, et al., 2021)
Fig.2 Role of IL-12 family cytokines in maintaining a balance between effector and regulatory immune responses in tumorigenesis. (Mirlekar B, et al., 2021)
IL-12 activates an effector immune response against tumor cells by promoting both M1 macrophage polarization and IFN-γ- production by Th1 cells, which in turn, stimulate anti-tumor cytotoxic CD8+ and NK cells. IL-27 and IL-23 have dual effects on immune cells in cancer. IL-27 and IL-23 can induce an overall T cell-mediated immune response and also modulate immune suppressive macrophages. Furthermore, IL-23 can stimulate the proliferation and growth of tumor cells. Conversely, IL-35 is a strong immune suppressive cytokine; it induces regulatory B and T cell activation and proliferation that subverts anti-tumor immunity and stimulates tumor growth and metastasis. IL-39 was recently shown to be secreted by B cells and may increase cancer cell proliferation. ↑ Arrow indicates increase in respective cell type activity; Tr1—T regulatory type 1; ILC—innate lymphoid cell; Breg—regulatory B cell; Treg—regulatory T cell; iT35— IL35-inducible regulatory T cell.
If you have any questions, requirements, or cooperation intentions, please feel free to contact us. We very much look forward to working with you and helping you achieve research and commercial success.
Related References:
- Gee K, Guzzo C, Che Mat NF, Ma W, Kumar A. The IL-12 family of cytokines in infection, inflammation and autoimmune disorders. Inflamm Allergy Drug Targets. 2009;8(1):40-52. doi:10.2174/187152809787582507
- Shimizu J, Kaneko F, Suzuki N. Skewed helper T-cell responses to IL-12 family cytokines produced by antigen-presenting cells and the genetic background in Behcet's disease. Genet Res Int. 2013;2013:363859. doi:10.1155/2013/363859
- Mirlekar B, Pylayeva-Gupta Y. IL-12 Family Cytokines in Cancer and Immunotherapy. Cancers (Basel). 2021;13(2):167. Published 2021 Jan 6. doi:10.3390/cancers13020167

